9am - 5pm EST M-F
9am - 5pm EST M-F

Osteoarthritis (OA) in the knees is a degenerative disease progressing through four stages, each affecting joint health differently. Recognizing these stages helps in seeking timely intervention and managing symptoms effectively.
Osteoarthritis, the most common form of arthritis, occurs due to the breakdown of cartilage, the protective tissue at the ends of bones in the joints. Over time, the wear and tear on cartilage can result in joint pain, stiffness, and swelling, making daily activities challenging. Factors contributing to OA include age, joint injury, repeated stress on the joint, obesity, and genetics. These elements can accelerate cartilage deterioration, leading to the early onset of OA symptoms.As OA progresses, it can cause changes in the bone and deterioration of the connective tissues that hold the joint together and attach muscle to bone. This degenerative process can significantly impact mobility and quality of life. However, early diagnosis and appropriate management strategies, including the use of knee braces, can slow the progression of OA, alleviate pain, and improve joint function. Braces specifically designed for OA can help by offloading stress from the affected joint, providing stability, and reducing pain during movement.
Braces play a crucial role in managing knee osteoarthritis by supporting the affected joint, promoting proper alignment, and distributing weight away from the damaged areas of the knee. They are particularly beneficial for individuals experiencing pain during activities such as walking, climbing stairs, or standing for extended periods. By stabilizing the knee and reducing the load on the joint, braces can help mitigate the symptoms of OA, enhance mobility, and improve the overall quality of life for those affected by this condition.

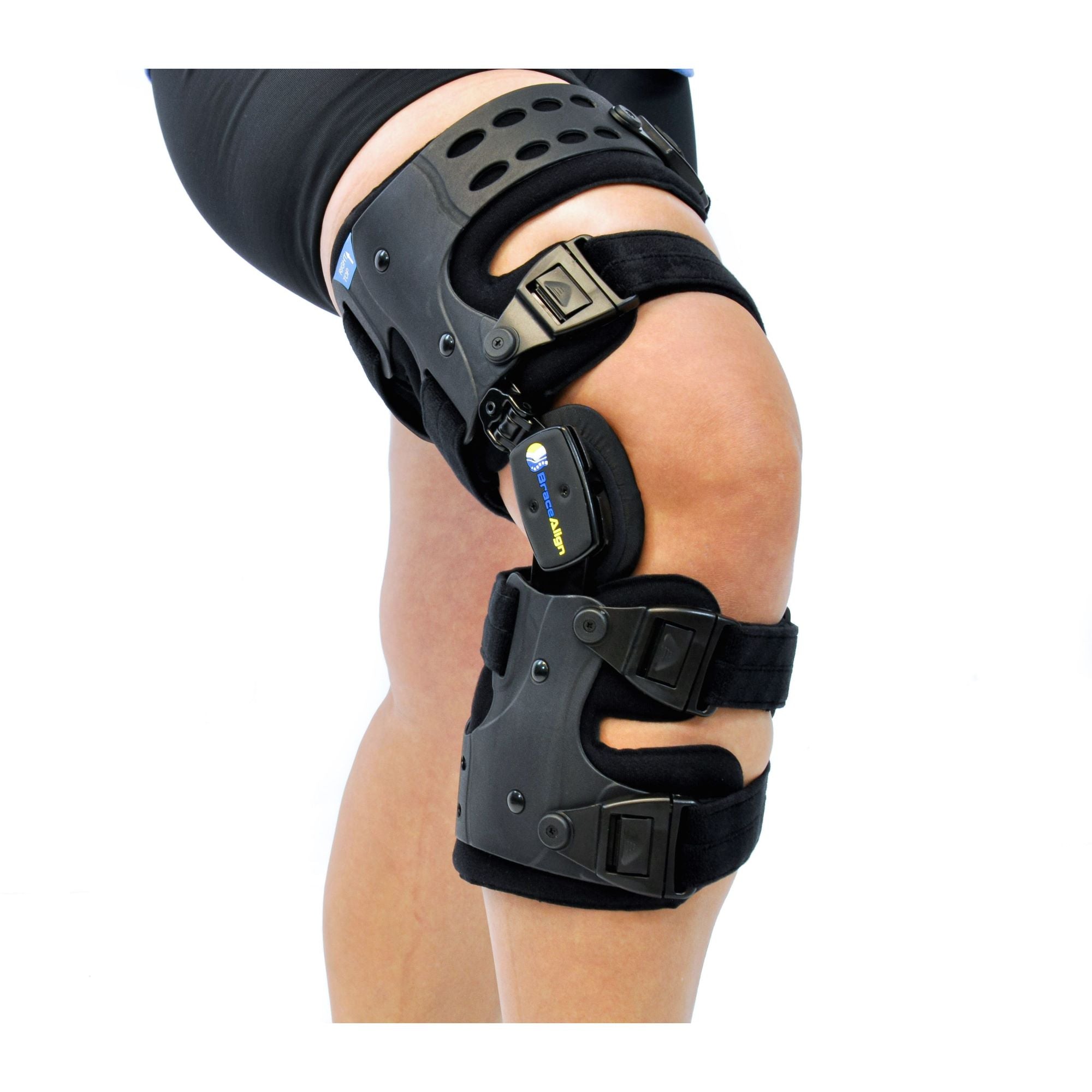
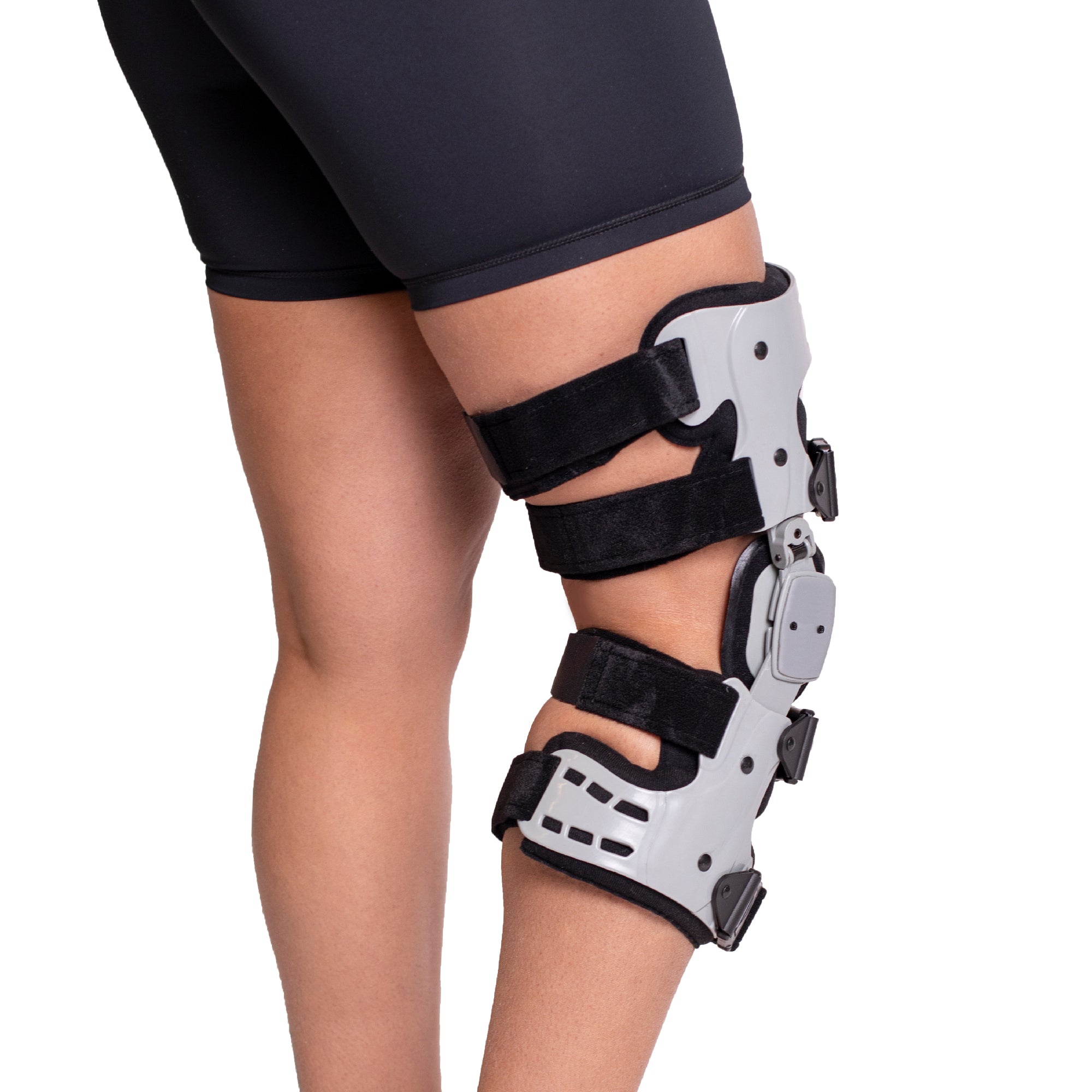

Proactively managing osteoarthritis involves understanding its stages, adopting lifestyle changes, and utilizing supportive devices like unloader braces. These measures can significantly improve quality of life and delay the progression of OA.